Osteoporosis is treated conventionally with a group of medications called bisphosphonates, like Fosamax, Actonel and Boniva. Unfortunately, these medications are not without serious risk. A letter published in the New England Journal of Medicine on January 1, 2009 by Diane Wysowski of the FDA’s division of drug risk assessment indicates a significant risk of lethal esophageal cancer. According to a Reuter’s report, “Wysowski said since the initial marketing of Fosamax, known generically as alendronate, in 1995, the FDA has received 23 reports in which patients developed esophageal tumors. Typically, two years lapsed between the start of the drug and the development of esophageal cancer. Eight patients died, she reported. In Europe and Japan, 21 cases involving Fosamax have been logged, with another six instances where Procter & Gamble’s Actonel or risedronate and Didronel or etidronate, and Roche’s Boniva (ibandronate) may have been involved. Six of those people died. Esophagitis, which is an inflammation of the lining of the tube carrying food to the stomach, is already know to be a side effect of the drugs, which is why patients are instructed to remain upright for at least a half hour after taking them.” Other significant risks associated with the drug are jaw necrosis (destruction of the jaw bones) and the potential of chronically irregular heartbeat (atrial fibrillation).
The concerns that have been raised regarding these medications have resulted in many women being hesitant to take them and looking for other treatment options. While these risks are quite serious, patients taking these medications should not discontinue without discussion with their physician. Depending on each patient’s individual circumstances, more comprehensive treatment plans can be considered. And if a prescription medication seems indicated, there are other measures you can take to prevent additional bone loss and perhaps augment the effect of the medication.
Increasingly, scientific studies are indicating that the same dietary habits that cause heart disease may also influence bone loss. The factors involved in bone metabolism are much more complex than just calcium and vitamin D. While these two nutrients are well known by the general public, many other adjustments to dietary intake can be made to reduce bone loss.
Researchers are now classifying osteoporosis as an inflammatory disorder, not just a disease of nutrient deficiency. Supplying nutrients alone is typically not effective enough to address the disease thoroughly. Factors involved in the inflammatory cascade include insulin which can be measured by a simple fasting blood test. If levels are elevated, addressing insulin resistance through a comprehensive treatment approach may influence the level of bone loss. For patients who have osteoporosis, I typically include insulin and inflammatory markers on the laboratory evaluation, as well as an NTX urine test to measure the current status of bone metabolism. This test can be used to follow-up on treatment earlier than the standard of care bone density test, which is typically not repeated for 1-2 years after starting treatment.
High protein diets are commonly used for weight loss. In osteoporosis, protein can influence how much bone is formed. Both the source of the protein and total amount of protein have effects on bone. The USDA’s Agricultural Research Service compared women who consumed purely plant based diets (vegan) versus mixed animal and plant based diets (omnivore). They observed the women who followed a vegan diet formed more bone but lost the same amount as the women consuming an omnivore diet. Bone metabolism is a balance between breakdown and building, so with respect to dietary protein source, the more plant based protein in the diet, the better. Also getting enough protein, but not too much, is important for bone health.
A study published in the American Journal of Clinical Nutrition in 2009 indicates a higher dietary intake of colorful vegetables and fruits may be protective against bone loss. A class of plant compounds called carotenoids (the most widely known is beta-carotene), are associated with reduced fracture risk in the elderly. Women consuming the highest amounts of lycopene, had a 2.5 fold reduced risk of fracture compared to women with the lowest intake, while in men the protective compounds were beta-carotene, lycopene, lutein plus zeaxanthin, and total carotenoids . Lycopene is commonly found in highest amounts in tomato sauce, watermelon, pink grapefruit and guava. To ensure a high intake of carotenoids, make sure your daily diet is rich in foods like sweet potatoes, carrots, squash, dark green leafy vegetables like kale, chard and spinach, avocado, apricots, mango and peaches. Other dietary recommendation that help prevent further bone loss include reducing sodium, caffeine, and carbonated beverages, all of which promote bone loss.
Finally, the importance of exercise cannot be underestimated. Particularly, weight bearing exercise is the form of exercise that “stresses” the bones enough to prevent bone loss. Performing load bearing exercises thirty minutes at least three times per week, especially before you are 25-30 years old significantly reduces the risk of osteoporosis. Types of exercise that are considered weight bearing are those that work your muscles against gravity like weight lifting, walking, aerobics, dancing, jogging and hiking. Once significant bone loss has occurred, some patients may falsely believe that exercise may be inadvisable. In most cases this is not true and your doctor can advise which forms of exercise will be most beneficial. Patients should check with a physician before starting any exercise program.
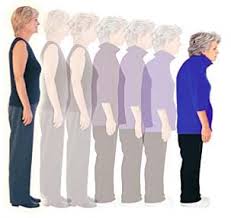
Rethinking Osteoporosis- Beyond Calcium, Vitamin D and Prescriptions